New fibre-optic technology could heal wounds faster
A new technique which delivers light deeper into human tissue than previously possible has been developed by researchers at the University of St Andrews and Harvard Medical School.
The new method, published in the journal Nature Communications, could help heal wounds faster and treat tumours more efficiently.
Through a process called photochemical tissue bonding, light is applied to a wound to stimulate healing. Until now this technique has been limited to treating superficial wounds. The researchers set out to develop a technology for tissue repair that would allow this method to be applied deeper in the human body.
The international team found a way to make biodegradable optical fibres which can be inserted into the body to deliver light to heal internal wounds locally, for example after surgery.
Traditionally, fibre-optic devices or catheters have been fabricated from glass or plastic and remain in the body permanently or until removed through further surgical intervention. However, the St Andrews-Harvard research team shows how fibres can be made from materials that will be reabsorbed into the body, eliminating the need for removal and the risk of damaging the newly-repaired tissue. This advancement will give doctors the power to heal from within without scarring.
Professor Malte Gather, of the School of Physics and Astronomy at the University of St Andrews, predicts that this breakthrough could have dramatic implications in medicine. He said: “A variety of optical techniques, such as photochemical tissue bonding and photodynamic therapy, require efficient delivery of light deep into tissues, but the current limited penetration of light in tissue constitutes a serious constraint in clinical use.
“Having biocompatible and bioabsorbable optical components may transform photomedicine from a discipline where light is predominantly applied externally, to a new paradigm based on tissue-integrated and precisely controlled delivery and collection of light.”
The research could also find application in a variety of other areas, such as long-term photodynamic therapy (PDT) for cancer treatment, as well as implanted endoscopy after surgery for repeated imaging and monitoring of the healing process.
Notes to news editors
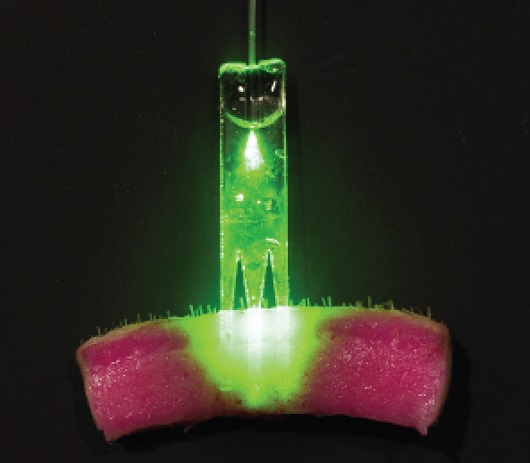
Image caption: ‘Bioabsorbable optical waveguides can be implanted into tissue to deliver light deeper and more effectively. After use, there is no need for removal as the waveguide disappears over time.’
The paper is available online at: http://dx.doi.org/10.1038/ncomms10374
Professor Malte Gather is available for interview. Please contact the Press Office on 01334 462 530 to arrange.
Issued by the University of St Andrews Communications Office, contactable on 01334 462530 or [email protected].
Category Research